Solving the Surgical Training Gap: Interview with Dr. Justin Barad of Osso VR
Published · Updated
Dr. Justin Barad speaks about the surgical training gap at NVIDIA Emerging Companies Summit 2016
Have you ever wondered how people get started in VR? Or more specifically – VR for healthcare?
Me too.
An interview with Dr. Justin Barad by Kristi Hansen Onkka
December 9, 2016
We all know surgical simulation for medical devices has always been an important part of surgeon education on new devices and techniques. Training for surgery is usually done on cadavers or on the job.
Today, virtual reality headsets offer a new way for surgical training. And a new way for medical device manufacturers to ensure their products are used properly and safely.
With any virtual reality experience, there are good ones and bad ones. Until now, surgical simulation was relegated to a few “alien-esque” experiences on Steam. Not exactly clinical utility at its finest.
Alien Surgical Simulator 2013.
But all that has changed with the launch of Osso VR. From their website: “Osso VR is an award-winning surgical simulation platform designed to train residents as well as enable more experienced surgeons to ‘warm up’ for their procedures. Our product offers highly realistic hand-based interactions in an immersive training environment.”
I was curious about the vision and mission of Osso VR. In my research, I found one differentiating factor that stood above the rest. Osso VR was founded by a pediatric orthopaedic surgeon.
Why would a surgeon decide to start a VR business?
Two weeks ago, I sat down to talk with Dr. Justin Barad, founder of Osso VR, who has not only worked in pediatric orthopaedic surgery at Boston Children’s Hospital, but was also a biodesign innovation fellow at Stanford Byers Center for Biodesign. In fact, one of the co-directors of Stanford Biodesign, Thomas Krummel, is on the Osso VR advisory board.

Dr. Justin Barad
Dr. Barad has a vision. A vision to help people.
From his early days as a biomedical engineering undergraduate at University of California, Berkeley, Dr. Barad knew he wanted to invent something that would change lives. His mentor, a gastroenterologist, told him that if he really wanted to know what type of invention was needed to help people, he should become a doctor himself.
So that’s what he did. In doing so he found a passion for pediatric orthopaedic surgery, helping children and their families. Dr. Barad not only enjoys helping kids, he likes the mechanics of the surgery itself. He is inspired by the advancing surgical technology used to fix and heal these young growing bodies.
As an orthopaedic surgeon, he has to keep up on the latest tools and techniques. While he got a lot of training throughout his residency, the extensive practice on one procedure or with a particular surgical device is limited. There isn’t enough time or resources to keep up. He noticed this in not only himself, but in his colleagues as well.
For instance, Dr. Barad recalls looking up instructions for use on a product website while talking a colleague through the surgical tool functionality during a procedure.
He mentions a couple of factors have created this void in surgical training.
One, there is a reduction in surgical hours. He says “the good thing is they get to sleep, the bad thing is there is less time for training and experience.”
In addition, “procedures are increasing in number. On top of that, they are becoming more complicated. They are adding navigation and robotics.”
Manufacturers help offset the learning curve on more complex devices by providing reps that help with procedures. Dr. Barad notes that surgical reps are a big help in the operating room, but even they need on-going training.
Enter Virtual Reality
At the same time he was finishing his residency, Dr. Barad tried out his first VR experience: the Tuscany VR Demo on the Oculus Development Kit 1. But it wasn’t until he tried the quirky and cartoonish Surgeon Simulator 2013, he knew VR was the platform for his invention that would help save lives.
He began teaching himself Unity with a vision to create a solution to this gap in surgical training. In February 2016, he met Matthew Newport, a veteran game developer and current CTO. Together they formed Osso VR.
The Osso VR Surgical Simulator launched in June 2016. And it has a lot of promise. With the more complex surgical environment, it is difficult to remember the tools and steps for a particular surgical procedure, even if a surgeon has been properly trained on it.
Dr. Barad believes Osso VR is effective as an introduction to a new device system or surgical technique, a refresher, or even as a warm-up for familiar yet complex procedures.
Osso VR can help device manufacturers create virtual surgical simulations to help augment real-world experiences. They can create medical procedure simulations that train sales reps, surgeons and the surgical staff in a variety of OR and patient settings. Dr. Barad even sees the potential of using this technology to better inform patient consent, or at least give a visualization of what to expect.
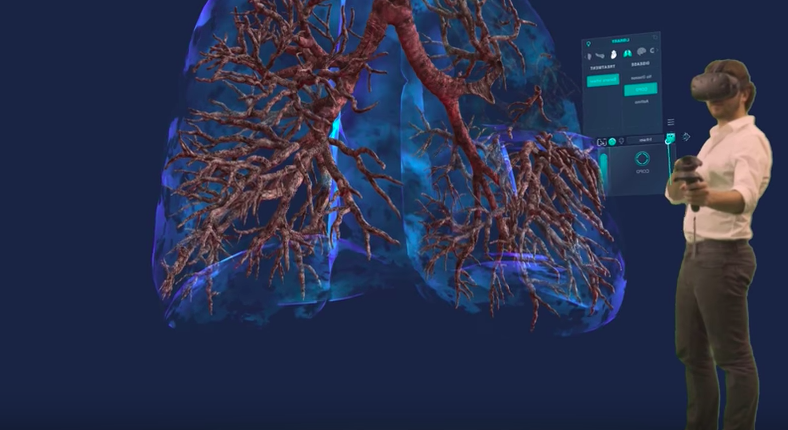
Using Your Hands
Osso VR builds surgical simulations for platforms that support high-fidelity hand tracking such as the HTC Vive and the Oculus Rift. This allows users to pick up and maneuver the surgical tools. The Osso VR development team spent a lot of time thinking about how hands would be visualized and used within the simulation.
Dr. Barad writes on Unity.com:
Our very first task was to decide how to represent hands in VR. Two popular options are having human hand models and animations like in Oculus’s Toybox Demo, or models of the controller such as in Tilt Brush. We ultimately decided upon having human hands as this felt more appropriate for a medical simulator.
The “human hands” coupled with handheld sensors provide simple haptic (touch sensitivity) feedback that Dr. Barad says is surprisingly satisfying for his tactile needs.
I was curious about that. I had always heard that smart and precise haptic feedback was crucial for any surgical simulation. Dr. Barad pointed me to a 2012 Study, “Perceiving haptic feedback in virtual reality simulators” that said otherwise. The study involved 20 surgeons using laparoscopic VR simulator with two handles. One handle had haptic feedback and one did not. “The surveyed surgeons believe that haptic feedback is an important feature on VR simulators; however, they preferred the handles without haptic feedback because they perceived the handles with haptic feedback to add additional friction, making them unrealistic and not mechanically transparent.”
In other words, it sounds like less haptics, counter-intuitively, might be better when it comes to surgical VR experiences.

Dr. Justin Barad on stage at the Exponential Medicine conference in October 2016
But is Surgical VR really accessible for surgeons?
We also spoke of access to VR technology. For example, the HTC Vive is not cheap. It runs about $800, and you need a high-powered computer (another ~$700) to run it. But, Dr. Barad, along with many in the VR community, sees the issue of access temporary. Prices will continue to drop in 2017 and new products will come on the market.
I was glad to hear that Osso VR is not letting access be a barrier. In fact, they are thinking about new technology and advances over the next year. Dr. Barad would not disclose any tidbits of what’s next for Osso VR, but my guess is we will see a lot more clinical innovation in the future.
In addition, Osso VR is an economical way for companies to create surgical simulation.
healthiAR featured post: Hands-On Surgical Simulation from Osso VR
Are you ready to fill your surgical training gap?
Osso VR is available to partner with device manufacturers looking to extend their training programs into the virtual reality space. Contact them at ossovr.com
Osso VR is featured on our infographic Your Human Journey: A Prescription for Virtual Reality. Check it out!

About Kristi Hansen Onkka
Kristi is the founder of healthiAR and is passionate about the impact virtual and augmented reality will have on healthcare. Visit her at getkristi.com.




What do you think?
4 Community thoughts on "Solving the Surgical Training Gap: Interview with Dr. Justin Barad of Osso VR"
[…] healthiAR featured article: Solving the Surgical Training Gap: Interview with Dr. Justin Barad […]
Fascinating interview! I really love that he learned Unity himself to start out. That’s super inspiring as I’ve been on the fence about learning it myself. Very cool that he’s using this new tech to solve the major problem of not enough time for good training.
[…] 2017 proved to show the clinical utility of VR in health. And what OSSO VR is doing for surgical training, Sim for Health is doing for practice training. Kristi Hansen Onkka […]
[…] to health. I also got to finally meet Justin Barad of Osso VR whom I had interviewed about using his VR technology to solve the training gap last month. In this video, he talks more about the excitement for health and VR. And, we get to see […]